The NHS, Triage and the Virus. Pt 1.
NHS England has long denied it rationed access to intensive care during the pandemic. However, as the current NHS crisis shows, questions about rationing and population triage refuse to go away.
On July 14, 2022, in the interregnum between Boris Johnson’s resignation and Liz Truss’s election as leader of the Conservative Party, a retired GP in Cornwall faced a life-or-death decision. For four days, Alison Durkin, who suffers from a narrowing of the arteries that supply blood to her heart, had been plagued by searing chest pains. Awakening in agony the previous Monday, Alison had called an ambulance and been taken to the Royal Cornwall Hospital in Truro. But there were no beds in A&E that day and after waiting six hours to be admitted, she was informed that her symptoms were most likely due to Covid-19 and sent home.
However, the next day Alison tested negative for Covid and her symptoms of ischemia worsened. Worried that his wife’s condition was becoming critical, Ross Durkin looked around for another hospital that might be able to admit her. But Britain was in the grip of a heatwave and because of staff absences and excess admissions due to the searing temperatures A&E departments across southwest England were oversubscribed. “We checked Plymouth, Exeter and Bristol but they were no better,” recalled Ross.
That left one option: London. Reasoning that Alison might have a better chance of accessing the urgent medical care she needed in the capital, Ross decided to drive her to Charing Cross Hospital, in Hammersmith, west London, a road trip of 285 miles.
The Durkins’ gamble paid off. On arrival at Charing Cross there was only one ambulance waiting outside and within twenty minutes Alison had been admitted to A&E and was being strapped to a heart monitor. Soon after, she was moved to the medical assessment unit where she was seen by a consultant cardiologist. She spent eight days at Charing Cross having a battery of tests, including a coronary angiogram to check whether she had blocked arteries, before being given a clean bill of health.
“At Charing Cross, they couldn’t wait to get her in the door,” says Ross. “At Truro they couldn’t wait to get her out the door and the next one in.”

The Durkin’s experience is a perfect example of the postcard lottery in healthcare in the UK. It is also a good example of the way that, whether by accident or design, scarce health resources– such as access to a heart specialist and expensive medical technology – are increasingly rationed by the NHS.
Although the NHS is supposed to be a universal service free to all at the point of delivery, rationing has been a fact of life since the services’ inception. This rationing takes many forms and is most apparent when the National Institute for Health and Care Excellence (NICE), the body that provides guidance on which medications and treatments the NHS should purchase, refuses to recommend an expensive new cancer drug on the basis that it’s of marginal benefit compared to cheaper, existing treatments (rationing by denial). Sometimes, health commissioners may make an exception and decide to authorise a new drug or therapy for a particular group of patients (rationing by selection). Alternatively, patients may be put off a service by making it difficult to access it (rationing by deterrence) or they may be shunted off to another institution, such as a local authority, for their medical care (rationing by deflection).
Waiting lists and queuing in ambulances outside A&Es - or the nine-hour wait inside A&E experienced this summer by the new health secretary Therese Coffey - are another form of rationing (rationing by delay), as is the erosion of services due to staff cuts and other austerity driven savings measures (rationing by dilution). But perhaps the most pernicious form of rationing is the kind that occurs at the hospital bedside when clinicians, often citing “medical considerations”, apply their own cost-benefit calculi to life-and-death decisions affecting patient care. In normal times, such rationing is hidden from view. But the coronavirus pandemic and the crisis currently engulfing the NHS have made these rationing decisions increasingly visible.
Covid-19 and “NHS Surge and Triage”
One of the biggest unanswered questions about the government’s management of the pandemic is whether at the height of the crisis, doctors, either acting independently or at the prompting of NHS hospital trusts, applied a form of rationing known as “surge triage” to prevent Intensive Care Units (ICUs) being overwhelmed by patients with severe breathing difficulties and other complications of Covid.
Pandemic planners had long anticipated that an outbreak of a novel respiratory virus might overwhelm the NHS. This is because ICUs in England & Wales typically operate at or near capacity and the NHS has just 4,000 critical care beds or 2.42 per 100,000 population – half the European average. This bed shortfall is matched by a shortage of mechanical ventilators – 8,175 in the UK compared to 25,000 in Germany. In addition, when the pandemic hit, the UK had a third fewer doctors than the EU average and 44,000 nursing vacancies (those vaccancies now stand at 47,000).
Recognising these capacity limits, during the 2009 swine flu pandemic the Department of Health produced a document setting out the principles for what it called “staged triage for critical care”. In essence, this recognised that were the NHS to run out of critical care beds, patients would be assessed for treatment on the basis of survivability, rather than need, using a scoring system known as SOFA (short for Sequential Organ Failure Assessment). Similar advice prioritising those most likely to survive treatment was issued in 2011 and 2013, albeit with the SOFA scoring system removed. This was followed in 2017 by the circulation of a confidential briefing paper by NHS England, headed: “NHS Surge and Triage”. Once again, this called for patients to be assessed on the basis of survivability, but this time clinicians would apply a utilitarian calculation taking into account the disease specialties most likely to be affected and the corresponding “lost years of useful life” (for instance, the avoidance of maternal and perinatal deaths was ranked highest, with 90,225 and 30,060 lost years respectively, followed by childhood asthma with 19,700 lost years).
Between 2017 and 2020, discussions about the ethics of population triage appear to have fallen into abeyance as Whitehall grappled with the challenges of Brexit, but in March 2020, as the NHS recorded the first deaths from Covid-19, the Chief Medical Advisor, Chris Whitty, revived the discussions by asking medical ethicists serving on a government ethics advisory panel to come up with yet another triage scoring system.
According to an investigation by the Sunday Times’s Insight team, the Moral and Ethical Advisory Group responded with a document entitled “Covid-19 triage score: sum of 3 domains” that, had it been followed, would have seen many people excluded from ICUs using a “clincial fraility scale” based on their age and pre-existing health conditions, such as hypertension, diabetes and chronic pulmonary disease.
This advice was no doubt well-intentioned. All health systems have finite resources and as populations age and the demands on those systems increase it is impossible to provide everyone with access to the same level of care. In such circumstances, some ethicists argue that the fairest way to allocate scarce health resources across populations is by prioritising those with the most Quality-Adjusted Life Years, or QALYs, left to them.[1]
However, using QALYs – or any other system that seeks to assign scores to particular patient groups and/or disease conditions – is ethically fraught as it inevitably means that elderly people and those with underlying conditions and/or co-morbidities stand to benefit less from life-saving interventions than younger and fitter members of the population. By removing the element of clinical judgement, such scoring systems may also lead to situations where patients are escalated for critical care even where they are unlikely to benefit.
In the event, NHS England maintains that the fraility scoring system was never activated because, unlike in Italy, England never ran out of critical care beds and everyone who needed intensive care was eventually able to access it. “There was categorically NO blanket national decision to refuse care to any group of people, including on the basis of their age,” said NHS England responding to the Sunday Times’s allegations.
Professor Sir Jonathan Montgomery, the panel’s co-chair, concurred, adding that although NHS England had asked the panel to draft a Covid-19 triage tool, in the event it was not needed and he and his fellow panellists had been stood down on 28/29 March 2020 “without DHSC [Department of Health and Social Care] or NHS implementation”.
“Decison-making” during pandemics
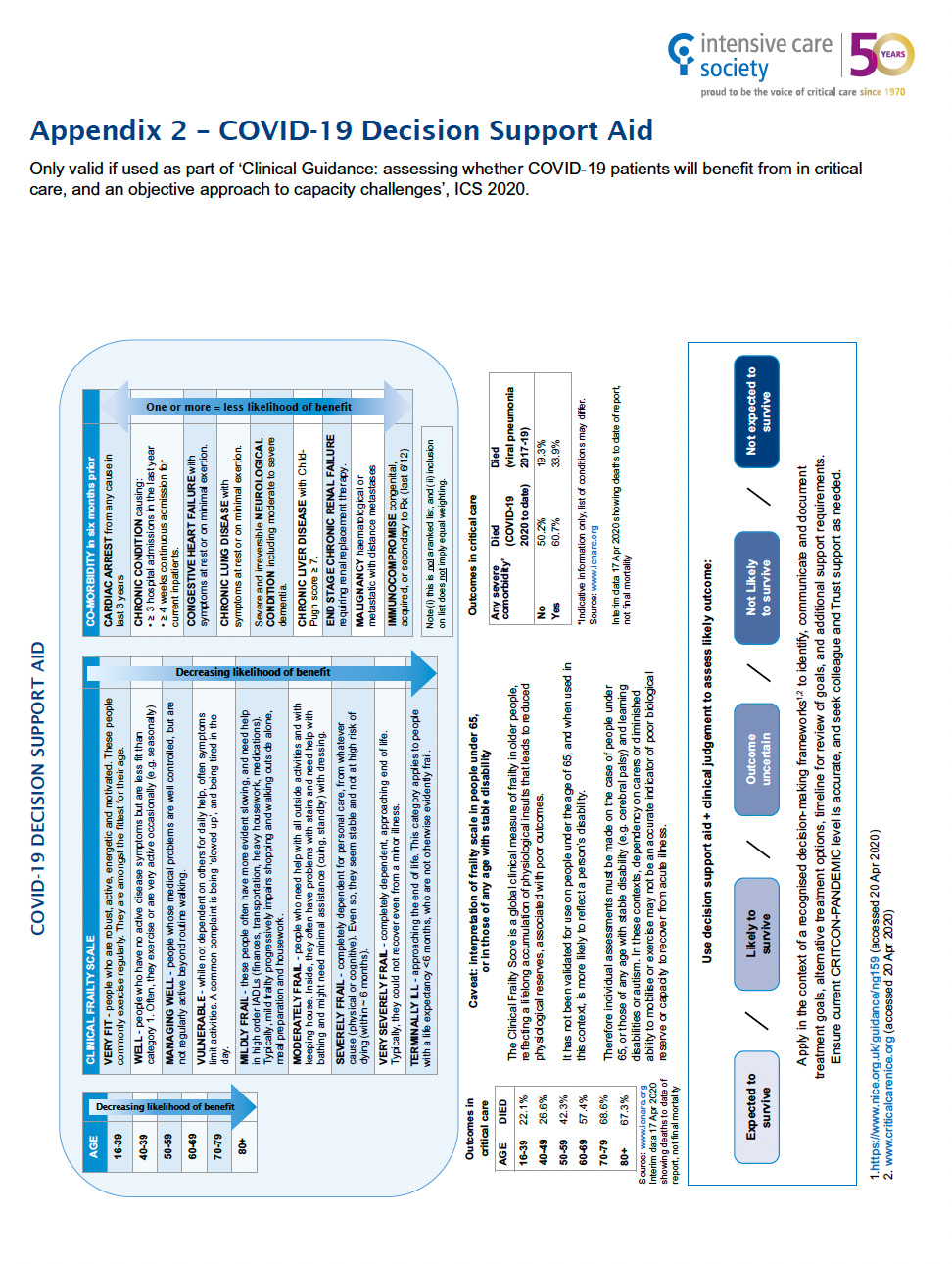
Nonetheless, in May 2020 the Intensive Care Society issued guidance for physicians working in intensive care “under pandemic conditions” stating that, although patients must be treated “without discrimination”, medical assessments could take into account such factors as “age, frailty and comorbidities”. The guidance was accompanied by a “Covid-19 decision support aid” containing a “clinical frailty score” and a list of pre-existing conditions, such as chronic lung disease and congestive heart failure, that, taken together, could decrease the “likelihood of benefits” to patients.
However, according to the ICS, implementation of the guidance was “the responsibility of individual trusts” and was desgined for “individualised” rather than population-wide decision-making. Only in the event of a “CRITICON PANDEMIC-4” surge could it be used to allocate resources “according to those patients most likely to benefit”.
For many doctors, including Dr Moosa Quershi, a consultant haematologist who has been campaigning for greater transparency on the UK’s preparedness for a pandemic, this is concerning as it leaves clinicians not knowing which guidelines to follow when resources are under severe strain and whether or not they will be held liable for decisions that should properly be the responsibility of NHS England and hospital trusts
“To this day I’ve had no official guidance on triaging in the event of a pandemic,” he told me. “That can’t be right. Doctors need clear guidance from the top, otherwise they run the risk of being held liable for resource allocation decisions that are outside their remit.”
… in Part 2 of this post next week, I examine the concerns of the Covid bereaved that life-saving treatments may have been withheld from their loved ones using triaging tools and inappropriate “Do Not Attempt Resuscitation” orders.
[1] The National Institute for Clinical Excellence (NICE) defines QALYs as “[a] measure of the state of health of a person or group in which the benefits, in terms of length of life, are adjusted to reflect the quality of life”.